We put our bodies under immense strain while training for and competing in trail races and ultramarathons. Time and again, our bodies exhibit what can only be described as remarkable adaptation to that strain. Many of these factors are environmental in nature, such as heat and altitude, both of which we’ve written about at length in this column. But what about the cold? Do humans have specific ways of handling cold weather? And what does that mean as you tackle cold-weather training and racing?
The answer is yes, we do adapt to the cold! Well, to a degree. In this article, we explore what the scientific literature knows about how the body reacts and adapts to being in cold environments. So, grab those hats and mittens and let’s get out there!

Jill Homer in the White Mountains of Alaska, in December of 2019, when the temperature was -50 degrees Fahrenheit. Photo: Jill Homer
The Nuts and Bolts of Thermoregulation
When compared to other mammals, humans are pretty maladapted to surviving and thriving in extreme and/or chronic (prolonged and/or repeated) cold. Yeah, that’s a fairly grim start, but nevertheless humans have developed numerous behavioral and physiological adaptations to mitigate cold exposure and to thermoregulate as needed. This means maintaining thermal balance by reducing how much heat is lost to the environment and by increasing heat production within the body (2).
Generally, we do a good job of this by utilizing behavioral thermoregulation, such as by building shelter, utilizing high-insulation clothing, and engaging in physical activity (1). However, these things are not always adequate and we sometimes become cold. When that occurs, physiological responses kick in to help us maintain thermal balance. Consider your brain, specifically its hypothalamus, to be your body’s thermostat. When there is a decrease in your peripheral temperature (the temperature of your skin) and core temperature, signals are sent to your hypothalamus that say, “We’re cold!” In response, you begin to vasoconstrict, or your blood vessels tighten and reduce blood flow and volume in your skin (1). Vasoconstriction is triggered when your skin temperature falls below 95 degrees Fahrenheit (35 Celsius), and its primary role is to help slow heat loss and protect your core temperature (1).
Shivering is additionally triggered by a fall in core temperature and consists of repeated involuntary muscle contractions usually starting with muscles in the torso and moving out to the limbs in order to create heat from metabolic work (1). Shivering, although highly effective for producing heat, varies in intensity depending on the severity of cold exposure and cannot last forever. In fact, I’ve witnessed people rescued from nights spent unintentionally out in the backcountry who were alive due largely to shivering but who also shivered themselves straight into rhabdomyolysis (muscle damage leading to renal and/or kidney complications).
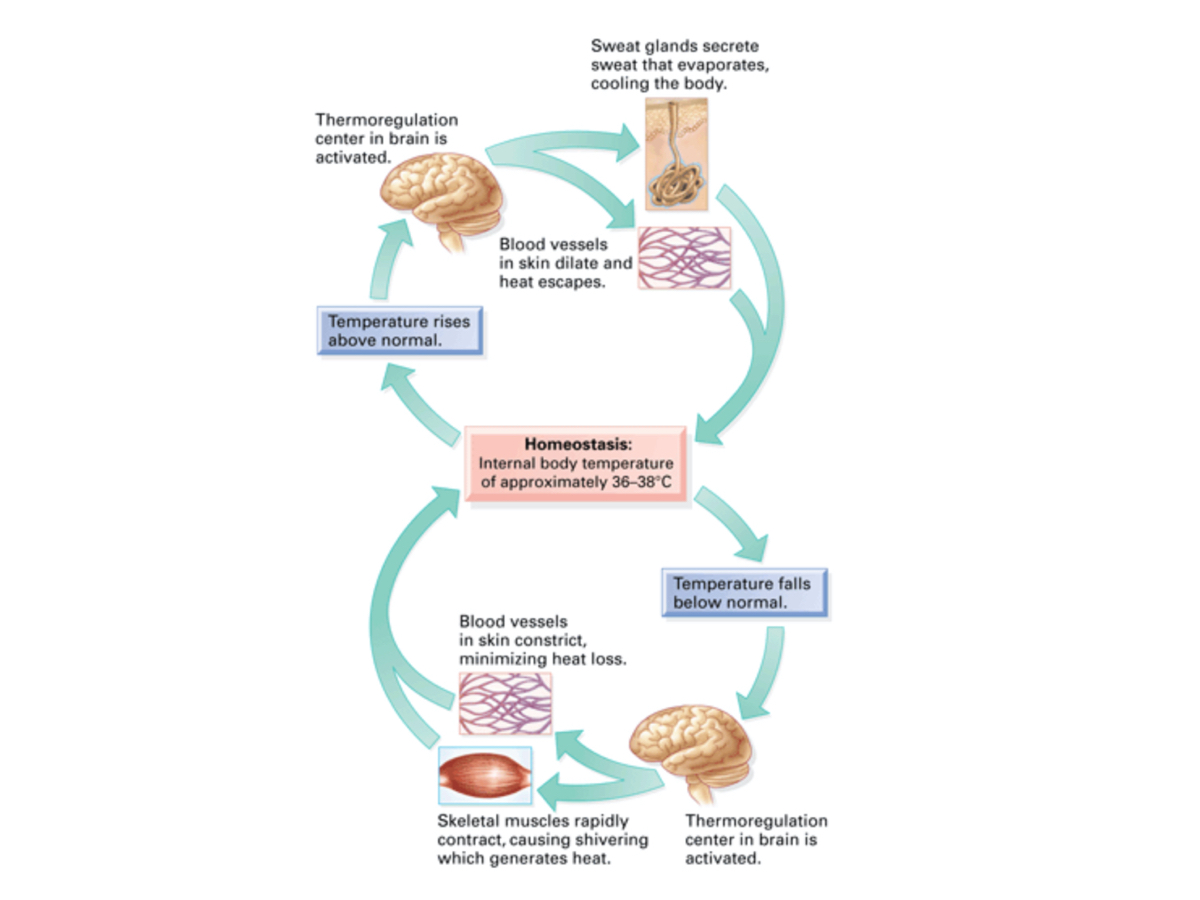
To maintain homeostasis, the brain acts as our thermostat. When we get too warm or too cold, it signals for minor adjustments to be made. Image: Ct-stem.northwestern.edu/curriculum/preview/170/page/1/
Cold Adaptation
Are there ways to truly adapt to the cold in a more long-term way? Indeed, with chronic cold exposure, three physiological adaptations take place: cold habituation, metabolic acclimation, and insulative acclimation (1). We will learn later in this article, though, that the degree of adaptation varies widely from person to person. But when combining these adjustments with proper behavioral choices such as layering, hydration, and nutrition, we now understand that you can feel comfortable as well as train and race well in fairly extreme temperatures. Let’s explore these physiological adaptations in detail.
Cold Habituation
The most common adjustment we make to chronic cold exposure is called cold habituation, or developing a decreased response to the cold. Specifically, our vasocontriction and shivering responses become blunted. This allows our core temperature to drop a little bit more than when unacclimated before we start to respond to the cold. Scientists believe this reduced response is linked to a decrease in norepinephrine, a hormone that triggers vasoconstriction, when exposed to cold. In a study where participants were exposed to 50-degree-Fahrenheit air for two hours a day, they saw a 20% decrease in norepinephrine response which in turn altered vasoconstriction (8).
Cold habituation is seen most regularly in both people who live in very cold environments, like circumpolar residents, and in those who have chronic cold exposure of relatively small areas of the body, like fishermen and fish filleters whose hands are immersed in cold water for long time periods (1). We also see this phenomenon in many of us “regular” folks, when we are chronically exposed to cold air or water.
Metabolic Acclimation
The next most common physiological adjustment is metabolic acclimation. People with metabolic acclimation have higher resting metabolic rates when in the cold. This allows them to maintain warmer skin temperature with less shivering when exposed to the cold (2, 3). This occurs via non-shivering thermogenesis, or heat production without active shivering.
While shivering relies on skeletal-muscle tissue, non-shivering thermogenesis relies on what is called brown adipose tissue (BAT). BAT is one kind fat tissue that is located in the interscapular (between shoulder blades), subscapular (beneath the shoulder blade), axillary (armpit), perirenal (around the kidneys), and periaortic (around the aorta) regions (6). BAT is primarily found around major arteries and veins, and it basically provides an internal heating jacket directly over your flowing bloodstream, warming it as it passes to and from your cooler peripheral regions (9). Although present in hibernating animals and infants, it was believed until about 10 years ago that adult humans didn’t have enough BAT to meaningfully contribute to thermogenesis (4). While adults have less BAT than when they were infants, we now know that this isn’t true.
White adipose tissue (WAT) is our more common fat tissue, and it’s located in most regions of the body. WAT’s roles are to store excess energy and provide some insulative warmth. And BAT’s role is to expend energy by metabolizing both glycogen (glucose) and lipids (fat) via oxidation, a process that literally creates heat. As you can imagine, there is currently interest in studying BAT and its role in non-shivering thermogenesis due to possible health implications such as weight loss and the management of type 2 diabetes (2, 3).
But back to cold adaptation. Can you increase your body’s BAT? It turns out that chronic mild to moderate cold exposure can increase BAT volume while decreasing your shivering intensity (2, 3, 4). Exposing your whole body to cooling via cold-air or cold-water immersion, however, is the most effective means of stimulating BAT volume and metabolism. There is still a lot of work being done in the scientific community on the appropriate dose, but it has been found that seven days of cold-water (57 degrees Fahrenheit) exposure for one hour a day or until the core temperature drops no more than three degrees (to about 95 degrees Fahrenheit) was effective for increasing BAT and its metabolic activity (2, 3). Cold exposure in general also appears to be effective, but over a longer time period. For example, running in the cold every day for 30 days also saw growth in BAT and an increase in its metabolic ability. Some of this appears to be seasonal acclimation, which means you may naturally regain BAT volume as the temperatures drop in the fall (7).
This is important for runners! This decrease in shivering intensity means you spare some glycogen that your muscles would utilize to create those muscle contractions, leaving it available as energy to fuel your workout.
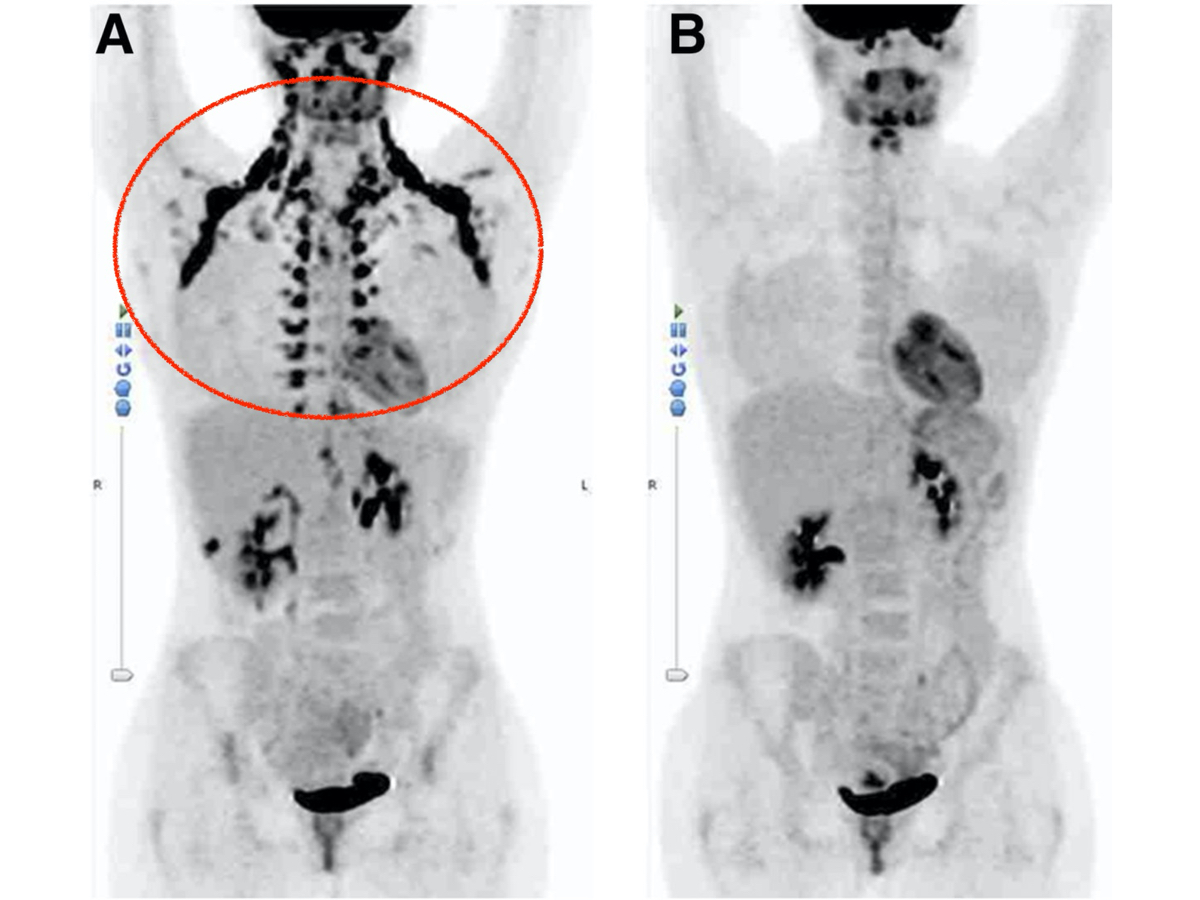
The area circled in red on the left positron emission tomography scan shows active brown adipose tissue (BAT), while the image eight days later after BAT minimization on the right shows little to no active BAT. Image: Jnm.snmjournals.org/content/59/8/1243/F4.expansion.html
Insulative Acclimation
The final physiological adjustment seen with chronic cold exposure is called insulative acclimation. This is the redistribution of blood flow utilizing the body’s own structures in order to keep the core warm, essentially enhanced vasoconstriction (1). What this looks like in a human with this insulative adaptation, like in the famously studied “ama” women of Korea and Japan who freedive without wetsuits in cold water, is an effectively maintained core temperature and cold-to-the-touch extremities (1).
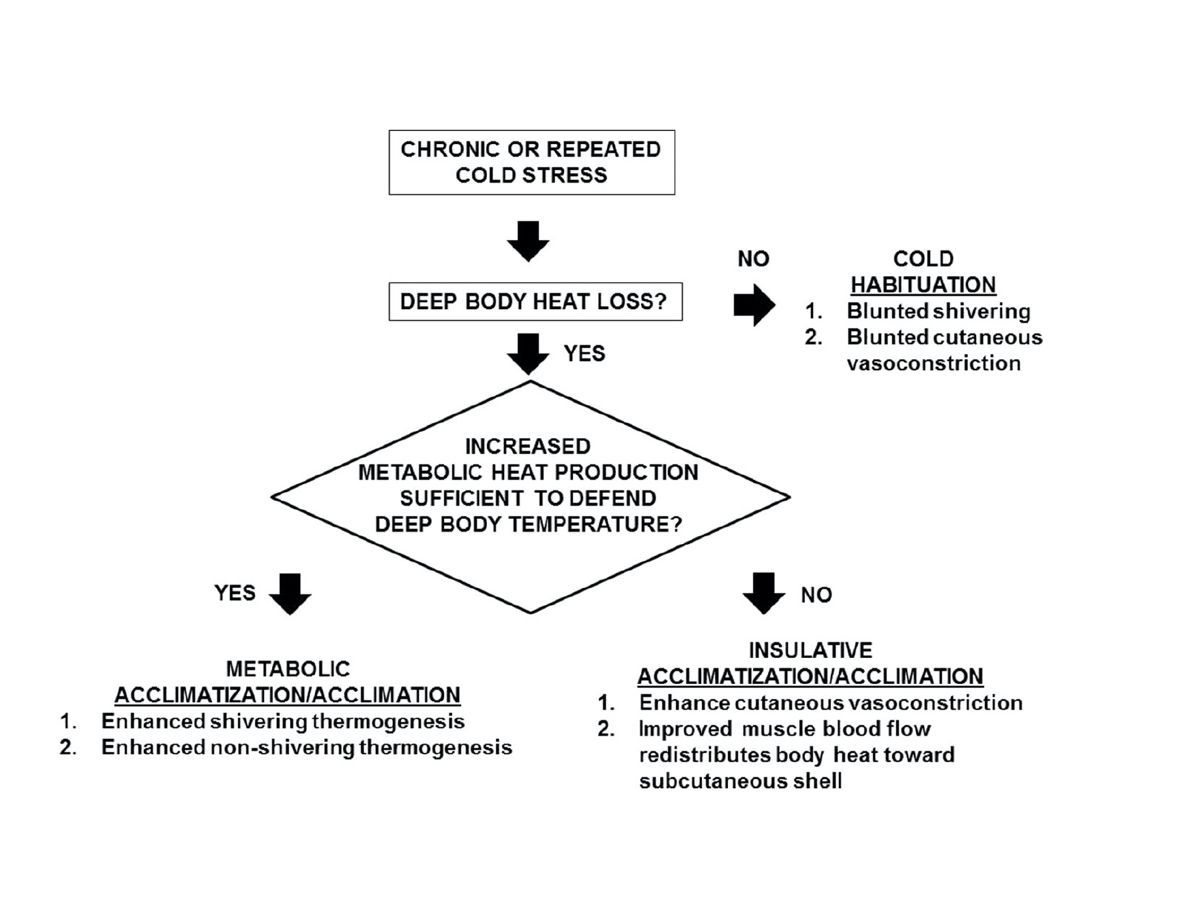
Three main physiological adjustments occur as a result of chronic cold exposure: cold habituation, metabolic acclimation, and insulative acclimation. Image: Castellani, J. W., & Young, A. J. (2016). Human physiological responses to cold exposure: Acute responses and acclimatization to prolonged exposure. Autonomic Neuroscience, 196, 63-74. doi:10.1016/j.autneu.2016.02.009 (1)
Cold Adaptation is an Individual Process
How well you adapt to the cold is unique to you. These are the factors that contribute to how we tolerate dips in temperature:
- Aging. We become less tolerant of the cold as we age, particularly as we cross the 60-year mark. This is largely due to our aging vasculature which reduces our capacity to vasoconstrict and thus conserve heat. Additionally, aging seems to reduce the core-temperature threshold at which vasoconstriction and shivering start (1).
- Gender. Gender plays a role in thermal sensitivity and managing thermoregulation, as seen in our article on Raynaud’s phenomenon. While we still have a lot to learn about the menstrual cycle’s effect on various physiologic processes, we know that body temperature/metabolic heat production varies across a woman’s cycle, with lots of individual variability. For example, women generally are less sensitive to shivering during their luteal phase compared to their follicular phase (1).
- Fatigue. When we get tired, we get bad at lots of things and that includes managing temperature. This blunted ability to manage temperature due to exertional fatigue is called thermoregulatory fatigue. When combined with multi-factor exhaustion, such as being underfed, sleep deprived, and physically exhausted (sounds like a long race, yeah?), we become much more susceptible to hypothermia (1). This is believed to be largely due to central fatigue and thus an inability to recruit skeletal muscles for shivering. Basically, you become so tired that you can no longer shiver enough to warm up.
- Fitness level. Endurance training might help keep you shivering, as we’ve learned through a study on mice. Shivering is a first line of defense for humans and mice against the cold, but as muscles fatigue, we have to rely more heavily on other ways to produce heat like non-shivering thermogenesis in BAT (5). Previous endurance training not only increases skeletal muscles’ ability to battle fatigue, allowing you to shiver for longer (endurance shivering for the win!), but it also potentially leads to the browning of white adipose tissue, allowing you to utilize non-shivering thermogenesis when you need it the most (5).
How to Increase Your Cold Adaptation
When winter sets in, there are a couple things you can do to make your outdoor explorations not only more comfortable, but also to help you perform better out there.
- Opt outside. You can gain cold adaptation from your day-to-day runs! Being exposed to even mildly cool air (below 50 degrees Fahrenheit) for two hours a day can create adaptation over the course of a month. Do keep in mind that there are temperatures that are unsafe for both cold injuries to your extremities and to your lungs (increased risk in developing exercise-induced bronchoconstriction), even with proper attire.
- Take the plunge. If you are looking forward to increased BAT and non-shivering thermogenesis, then whole-body cold exposure might be for you. The best way to do this is by cold-water immersion. Hello cold showers or ice-tub dunks! Exposing your whole body to cooling, although unpleasant, is the most effective means of stimulating BAT volume and metabolism. Take note that here is still a lot of work being done in the scientific community on this topic. For example, how this decays (loss of adaptation) over time or how you postpone that decay remains unclear and warrants future research.
- Keep running! Endurance exercise seems to do a few things to help us stay warm. Remember, endurance exercise in the cold can stimulate BAT growth and development and facilitate our cold habituation. This improves our non-shivering thermogenesis, vasoconstriction response, and spares glycogen by not having to rely on shivering for warmth. Additionally, endurance exercise has been shown to actually prevent possible “shivering fatigue,” or our muscles getting too tired to shiver in order to create heat. Keep running, because it can literally keep you warm!
Call for Comments
- Do you think you experience cold adaptation?
- And, do you think you “lose” your cold adaptation after a period of time when you aren’t exposed to it?
- Leave a comment to share your experiences about getting used to cold temperatures.
References
- Castellani, J. W., & Young, A. J. (2016). Human physiological responses to cold exposure: Acute responses and acclimatization to prolonged exposure.Autonomic Neuroscience, 196, 63-74. doi:10.1016/j.autneu.2016.02.009
- Gordon, K. E. (n.d.). Metabolic and Thermal Responses to Short-term, Intense Cold Water Acclimation Protocol.Department of Human Kinetics, Faculty of Health Sciences, University of Ottawa, 1-83. MSc Thesis
- Gordon, K., Blondin, D. P., Friesen, B. J., Tingelstad, H. C., Kenny, G. P., & Haman, F. (2019). Seven days of cold acclimation substantially reduces shivering intensity and increases nonshivering thermogenesis in adult humans.Journal of Applied Physiology, 126(6), 1598-1606. doi:10.1152/japplphysiol.01133.2018
- Blondin, D. P., Daoud, A., Taylor, T., Tingelstad, H. C., Bézaire, V., Richard, D., . . . Haman, F. (2017). Four-week cold acclimation in adult humans shifts uncoupling thermogenesis from skeletal muscles to brown adipose tissue.The Journal of Physiology, 595(6), 2099-2113. doi:10.1113/jp273395
- Knuth, , Peppler, W., Townsend, L., Miotto, P., Gudiksen, A., & Wright, D. (2018). Prior exercise training improves cold tolerance independent of indices associated with non-shivering thermo-genesis. Journal of Physiology, 596(18), 4375–4391. https://doi.org/10.1113/JP276228
- Carpentier AC, Blondin DP, Virtanen KA, Richard D, Haman F and Turcotte ÉE (2018) Brown Adipose Tissue Energy Metabolism in Humans. Front. Endocrinol. 9:447. doi: 10.3389/fendo.2018.00447
- Nishimura, T., Motoi, M., Egashira, Y. et al.Seasonal variation of non-shivering thermogenesis (NST) during mild cold exposure. J Physiol Anthropol 34, 11 (2015). https://doi.org/10.1186/s40101-015-0051-9
- Leppäluoto, J., Korhonen, I., Hassi, J., 2001. Habituation of thermal sensations, skin temperatures, and norepinephrine in men exposed to cold air. J. Appl. Physiol. 90, 1211–1218.
- Harold Sacks, Michael E. Symonds. (2013). Anatomical Locations of Human Brown Adipose Tissue: Functional Relevance and Implications in Obesity and Type 2 Diabetes. Diabetes. 62(6): 1783–1790. Published online 2013 May 17. doi: 10.2337/db12-1430

