Scenario 1:
You’re pacing your friend at the Rocky Raccoon 100 Mile. It’s her first 100 miler, and you’re excited to help her get her first big belt buckle. You finally spot her coming into the Damnation aid station at mile 60. You holler, “Hey there! Looking good! What can I get you?” She answers, “I’m not sure what’s going on. My chest, back, neck, and arms started itching about an hour ago. It’s driving me crazy. Look at my arms.”

An example of hives on an arm. Photo: AdaMacey
Her back and neck are also covered with hives. “What do you think I should I do?” she asks.
Question: What should you do?
A. Give her a Benadryl from your first-aid kit.
B. Wash the affected skin with water from the aid station.
C. Wait to make a decision until the next aid station in 4.5 miles.
D. Gather more information.
Answer: D. Gather more information.
You don’t know much of anything right now. Did your friend eat something she was allergic to? Did she run through something that might have caused the reaction? Has this ever happened before? What happened last time? Does she have an epinephrine auto-injector, like an EpiPen? Has she ever had to use it? Where is it? What exactly happened before she started itching? The answers to these questions will help you make a good decision about what to do next.
The SAMPLE mnemonic is a good way to remember the questions that will help you make a good decision about the best way to help your friend. This mnemonic is commonly used by emergency medical professionals:
S – Symptoms
A – Allergies
M – Medications
P – Past medical history
L – Last ins and outs
E – Events leading up to the illness or injury
When you ask your friend these questions, here’s how they answer:
S – Symptoms: Itching on chest, back, neck, and arms.
A – Allergies: Shrimp and scallops. She says, “I didn’t eat either of these during the race.” She doesn’t have an EpiPen.
M – Medications: None
P – Past medical history: None
L – Last ins and outs: She’s eaten and drank bananas, peanut butter and jelly squares, Nuun tablets, Velveeta grilled-cheese sandwich, and Tailwind. She hasn’t vomited and she urinated two hours ago.
E – Events leading up to the illness or injury: Her arms started itching after mile 45 (it’s mile 60 now) and the itching has spread slowly to her chest, back, and neck. She hasn’t eaten anything new besides the Velveeta. No shrimp or scallops at the aid stations. She’s stayed on trail and hasn’t run through any grasses or foliage.
So now what should you do?
Allergic reactions happen when your body decides it doesn’t like something like peanuts or bee venom. When it’s confronted with that thing, it releases the chemical histamine. Histamine can cause a whole slew of symptoms including:
- Runny nose or watering eyes
- Flushed and itchy skin
- Hives and/or welts on the skin
- Nausea
- Large areas of swelling
- Difficulty swallowing
- Respiratory distress
- Abdominal pain and vomiting
- Shock
The severity of the symptoms depends on how much histamine is released. Here’s an example of a mild allergic reaction (where a mild or moderate amount of histamine is released):
Body: I hate and fear peanuts! If she eats a peanut, there’s going to be trouble.
Runner: Eats bar with peanuts.
Body: Release the histamine!
Runner: Experiences flushed and itchy skin.
Here’s an example of a severe allergic reaction (where a large amount of histamine is released):
Body: I HATE AND FEAR PEANUTS! If she eats a peanut, there’s going to be BIG TROUBLE.
Runner: Eats bar with peanuts.
Body: DUMP THE HISTAMINE!!! DUMP IT!! NOW!!!!!! AHHHHH!!!!
Runner: Experiences respiratory distress and large areas of swelling.
The body can overreact and dump histamine in response to anything–foods, pollens, animal dander, plant oils, insects, drugs, cold temperatures, and even exercise. (I kid you not; there are people who are legitimately allergic to running.) So the treatment for a troublesome histamine release is, wait for it… an ANTIhistamine. Benadryl is a common antihistamine.
For a mild or moderate allergic reaction like your friend’s, an antihistamine will block the histamine and the symptoms will subside. If you can identify the cause of the allergic reaction, make sure to remove it. (No more mussels on the half shell at the aid stations for you!)
Treatment for mild/moderate allergic reactions:
- Remove the allergen or remove the patient from the environment with the allergen.
- Administer oral antihistamines.
- Monitor closely for facial swelling and respiratory compromise.
Because the body can continue to release histamine, it’s important to keep watching your friend to make sure she doesn’t develop any facial swelling or trouble breathing. We’ll get to how to treat a severe allergic reaction shortly.
For runners, especially runners in a long race, it’s important to know that antihistamines can have some troublesome side effects. Common side effects of antihistamines include:
- Dry mouth
- Drowsiness
- Fatigue
- Dizziness
- Disturbed coordination
- Upset stomach
- Blurred vision
The scenario continues:
After your friend takes an antihistamine, her itching subsides and the hives disappear. She’s close to cutoffs, but it seems like she’s going to be able to finish the race. But then she starts having to go to the bathroom frequently. After the fifth stop to pee in 90 minutes, you tell her she should stop drinking so much. “I know, but my mouth is so dry,” she tells you. Maybe it’s the antihistamine making her mouth dry. You tell her to try swishing the water around in her mouth and spitting it out instead of drinking it. The approach works, and she finishes the race.

Your friend finishing the Rocky Raccoon 100 Mile after recovering from a mild allergic reaction. Photo courtesy of Liza Howard.
At the hotel later that night, while she’s admiring her new belt buckle, the hives reappear. Happily, you’d stopped at the drug store before dropping her at the hotel to pick up more antihistamines. She takes another, and the hives subside for good.
Scenario 2:
You’re volunteering at an aid station and there are bees everywhere. They are on the orange slices, on the peanut butter and jelly sandwiches, and swirling around the spigot of the drink coolers.
You’re just removing a drowned bee from a cup of Coke when the volunteer next to you says, “Ah! It stung me!”
She was stung on her hand. Almost immediately, her hand starts to swell. Welts appear on her arm, and then her neck. “My throat feels itchy,” she tells you. There are no medical personnel at this aid station and no one with more knowledge than you.
Question: What should you do?
A. Give her an antihistamine from the aid station first-aid kit.
B. Gather more information.
C. Ask to see if anyone has an auto-injector of epinephrine, such as an EpiPen, Auvi-Q, or Adrenaclick.
D. Call 911.
Answer: B. Gather more information.
Using the SAMPLE mnemonic will help you get the information you need to treat this reaction effectively and as quickly as possible.
S – Symptoms: Itching on hand, arm, and in throat. “It’s feels harder to swallow,” she says.
A – Allergies: None. Nothing like this has happened before. Does not have an EpiPen or any antihistamine.
M – Medications: None
P – Past medical history: None
L – Last ins and outs: She had lunch. She urinated and had a bowel movement this morning.
E – Events leading up to the illness or injury: Was fine until stung by the bee.
These questions will take less than a minute to ask.
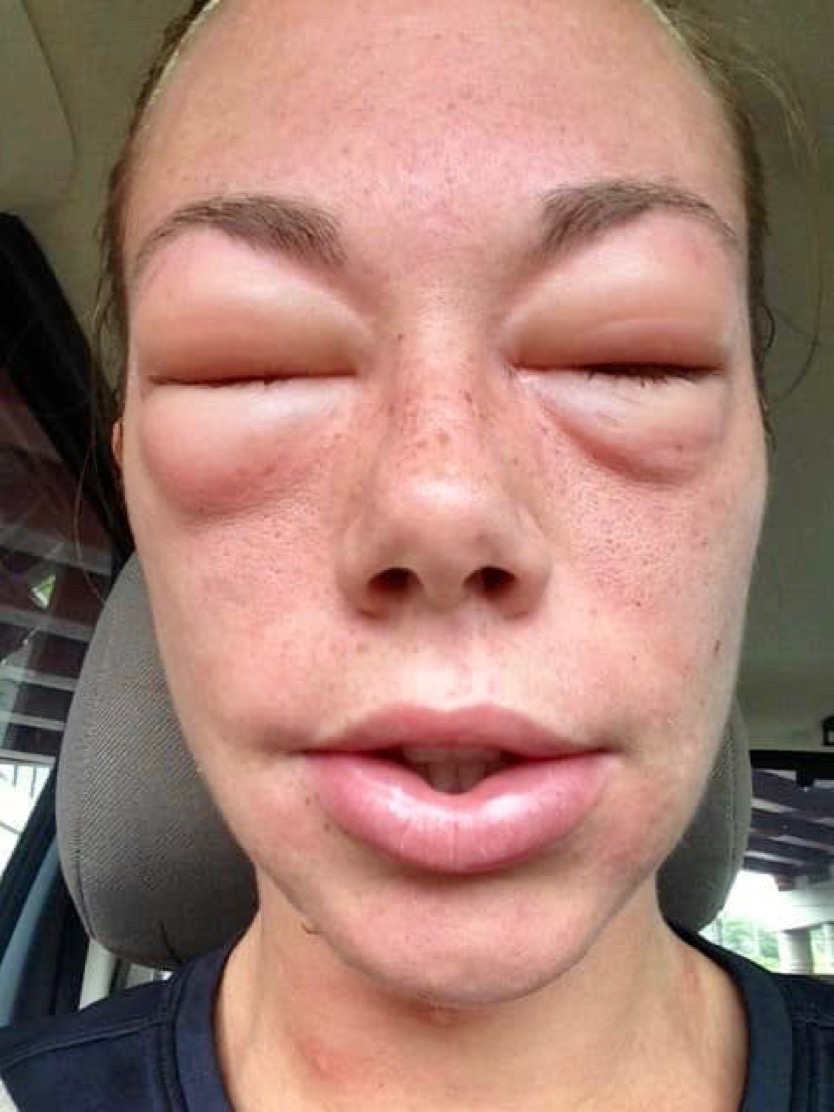
A large amount of histamine has been dumped into this woman’s system. Any reaction involving the airway or face, lips, and tongue is very serious. The swelling might compromise her breathing. Furthermore, large amounts of histamine can cause the blood vessels to expand and leak. That could lower her blood pressure enough that oxygen won’t be delivered to her cells. She’ll go into shock and potentially die. So, yeah, this is an emergency that requires immediate treatment. A severe allergic reaction like this is called an anaphylactic reaction.
She needs an antihistamine, but she also needs something that will open her airway passages, constrict the dilated blood vessels, and stabilize the cells that are releasing histamine and chemicals like it. That is what epinephrine does. This woman needs an injection of epinephrine along with an antihistamine.
You have neither. There’s no antihistamine in the first-aid kit, and no one at the aid station has any. There are no epinephrine auto-injectors either. You need to get this woman to medical help as quickly as possible. Calling the race director or whomever the race has identified as the person in charge of medical will get you that help faster than calling 911 in most situations.
Treatment for severe allergic reactions:
- Inject epinephrine with any airway swelling (lips, tongue, uvula, voice changes), large areas of swelling, and/or difficulty breathing or shock.
- In addition, whenever the patient is able to swallow, administer oral antihistamines.
- If reaction reoccurs, continue to administer epinephrine.
- Evacuate.
The scenario continues:
You call the race director and explain that a volunteer is having a severe allergic reaction to a bee sting. She tells you she’ll call 911 and that it’ll be quickest if you drive with the patient to the Donut Hole aid station to meet the ambulance. By the time the ambulance arrives 15 minutes later, the woman’s lips are swollen and her eyes have swollen shut.
The paramedics administer epinephrine and an antihistamine and transport the volunteer to the hospital. She recovers fully. Her doctor prescribes an auto-injector and tells her to carry it with her when she’s outside and to use it if she experiences similar severe symptoms. Sometimes people who have severe allergic reactions are told to use their auto-injectors as soon as they are exposed to a particular allergen because it’s so likely they’ll have a severe response.
Scenario 3:
Same volunteer. Same race a year later. Same bees. She’s stung and begins to have the same severe reaction. She reaches into her backpack and pulls out her EpiPen and injects herself. Here are videos showing how to use an EpiPen, Adrenaclick, and Auvi-Q.
Then she takes Benadryl (diphenhydramine) and asks you to drive her to the hospital. Anyone who receives an epinephrine injection needs to go to the hospital to be evaluated regardless of whether the symptoms subside. Severe allergic reactions are not one-shot deals–so to speak. The symptoms can return without re-exposure to the allergen over the next 12 to 24 hours.
The laws about using epinephrine auto-injectors vary from state to state and country to country. Californians can get a certification that will allow them to get an auto-injector to use on someone else who is suffering from a severe allergic reaction. In Texas, using your EpiPen on someone else is illegal. Look up the laws that apply to you. Antihistamines do not require a prescription and can be used as directed on the packaging. Race directors should have a plan for dealing with severe allergic reactions and make sure volunteers know what it is.
There’s no way you’ll remember the SAMPLE patient-history mnemonic if you find yourself needing it tomorrow. Take a Wilderness First Aid course to get more practice with it and buy a first-aid pocket guide that you can pull out when you’re caring for someone with a medical emergency.
[Author’s Note: Learn more about caring for allergic reactions and other wilderness first-aid skills with a two-day NOLS course. Thank you to Tod Schimelpfenig, NOLS Wilderness Medicine’s Curriculum Director and author of NOLS Wilderness Medicine, for his guidance and oversight of this series. Thanks also to graphic artist Brendan Leonard, the trail and ultrarunner of Semi-Rad fame, for his graphics collaboration in this article series.]
Call for Comments
Please share your story about an allergic reaction on the trail!

Image: Semi-Rad/Brendan Leonard