This past month, I ran across an insightful handout displayed at the Johnson & Johnson Physical Therapy clinic in Steamboat Springs, Colorado, my manual-therapy certification testing site. In an increasingly specialized world of medical care, it is increasingly common for clinicians to post a list of ‘what we treat.’ Atop the list posted at J&J is the ‘whole person.’ It sounds tongue-in-cheek, but the meaning is earnest. In order to achieve sustained recovery and optimal function, we must address the whole person and the whole system.
As such, when I provide free injury consults at my favorite running shop in Eugene, Oregon, Run Hub, each month, I struggle to provide quick-fix guidance to runners in need. Too often, pesky injuries–those that fail to spontaneously heal or fail to heal with conventional treatment–require a comprehensive, whole-person approach that goes beyond a quick, pop-in discussion.
That’s the buzzkill: quick fixes are rare. Too often, the quick-fix approach can devolve into a frustrating game of injury whack-a-mole, with a different injury replacing the one before it. However, comprehensive treatment doesn’t always have to be complicated and labor-intensive. A good roadmap to the whole person can illuminate the path to sustained healthy and fast running.
It’s All Connected!
To begin, we runners and the medical practitioners who treat us must accept the notion of interconnectedness. Even if we conceptually understand this, the idea can still seem really intangible. Yes, the ‘knee bone is connected to the thigh bone,’ but how all the body parts actually interact with each other can be elusive to most clinicians, let alone runners.
After a period of tremendous specialization, sports medicine and orthopedics is coming back to the notion of interconnectedness, calling it “regional interdependence.” This is the medical profession’s acceptance, after years of stubborn specialization, that we need to treat more broadly. Specific treatments depend on the person, but I’d like to present a simple outline of how components are connected in our running system as well as how and why we must address them for specific injuries.
The Systems Continuum
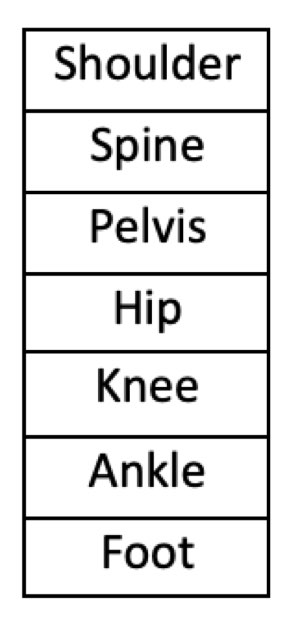
Below is a simplified physical continuum of body systems and their interconnectedness presented vertically, like the body:
Note that the spine should be subdivided into lumbar, thoracic, and cervical, with cervical above the shoulder. For simplicity, they are lumped into ‘spine’ and placed below the shoulder.
These motion systems are connected not just structurally but also in function. And the closer their proximity, the more impactful a dysfunction in one area can be on its neighbor. For example, it’s quite possible and often likely that a runner with knee pain also has dysfunction immediately above or below the knee, at the hip and/or the ankle. Beyond that, the foot and pelvis can also house dysfunctions which create and sustain knee pain. Thus, if that knee pain is being driven by impairments from above or below it, in many if not most cases, no amount of focal knee treatment will alleviate it. Indeed, the most chronic pain cases often have dysfunctions at every level in the system and the whole mess needs to be treated!
Lastly, a note on right and left, what happens on the right side impacts the left, and vice versa. Running is like the legs playing catch with the body. The right leg throws (push-off) and the left leg catches (landing). Then the left leg throws (push-off) while the right leg catches (landing). As such, a push-off problem on the right side invariably creates increased stress upon landing on the left side, and so forth. Thus, a unilateral injury requires addressing any inefficiency in the other leg.
So while it may seem complicated, complete recovery often depends on such comprehensive care. And for the runner, paying attention to minor and seemingly unrelated issues may be the key to pain relief as well as the prevention of stubborn injuries.
Sweat the Small Stuff
An interesting recent patient of mine highlights the big challenge and even bigger payoff of a whole-person treatment approach. A masters-age runner presented with chronic right hip and back pain. Her hip hurt intermittently, partially impacting running but was more painful with prolonged standing at work and home. Conventional, specialized treatment–isolated to the right hip and pelvis–had provided only temporary relief.
In the first-visit interview, she noted in her history a recent foot surgery to correct a bunion deformity and pain in her left first big toe. That toe feels better, but she continues to have pain in the other toes of her left foot. In watching her run, there is a clear push-off deficit in her left leg where the left foot rotates out and the left hip fails to extend as far or powerfully as the right hip. As such, her trunk leans right upon landing on the right leg.
While we did treat the range-of-motion loss in her right hip and low back, the key was treating her left foot and ankle. Improving mobility, strength, and push-off function in her left foot made an immediate difference in her gait. We then treated both sides of the pelvis via improving range of motion and strength adjacent to the hip. In a short time, we decreased her right hip and back pain by about 50%.
At the third visit, we began to address the next layer, the left knee. Upon further examination, the knee showed significant inefficiency with rotational torsion, where the tibia bone rotated too much externally while the femur rotated internally. As we began treatment, she added, “I’ve had left knee pain for years, and sometimes it gives out on me when running.”
This is what I call an oh-by-the-way moment, something a runner doesn’t tell you because they feel it’s irrelevant to their pain. Patients often believe that minor aches and pains (no matter how chronic) aren’t a big deal and are unrelated to the current and often more acute/impactful pain. Yet this ‘small stuff’ may loom large in a connected system and a whole-person treatment paradigm!
Indeed, treating the left knee resulted in full pain relief in the right hip. Ironically or not, very little direct treatment of the right hip and lumbar back was necessary.
To review:
- Treating the left knee improved the left-foot function.
- Treating the left foot improved left-hip function.
- Treating the left leg abolished the original complaint of pain in the right hip.
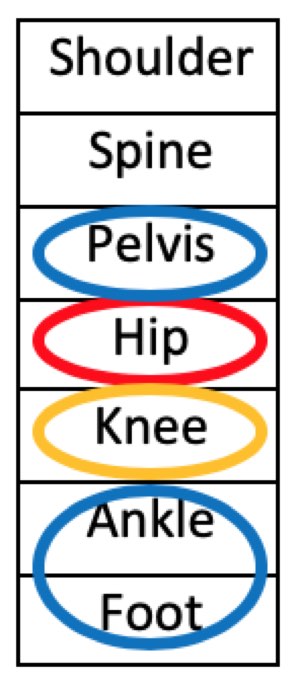
Here is a regional-treatment paradigm for this runner, with the tiers of treatment circles color-coded. Red indicates the primary dysfunction, blue is secondary/first tier, and yellow is second tier:
Conventional orthopedics and sports medicine are hyper-focused on the red circle, the focal painful area. Indeed, great medical advances have occurred in the skill and speed of treating the primary red-circle issues. Yet more often than not, complete recovery requires treating multiple levels of dysfunction. As I tell my patients, it’s simple but it’s not easy. Whole-person treatment is more work but it results in vastly superior recovery outcomes.
The Runner’s Take-Home Message
The important take-home message for the runner is not the importance of knowing the exhaustive specifics of every bone and joint in the body. Instead, it is that complete injury care and prevention depends on the recognition of regional interdependence and how small issues in one area can impact others and how these issues in other seemingly unrelated areas can create stubbornly painful dysfunctions anywhere else in the body.
The specific takeaways:
- Recognize that it’s all connected. Stiff hips or weak feet shouldn’t be blown off. Do your best to shore up any weak, stiff, or otherwise inefficient areas.
- There’s no such thing as a minor injury. Injuries are the result of a dysfunction in the system and can propagate dysfunction throughout the rest of the system. Do your best to address the small stuff before it grows larger or spawns more injuries.
- Demand whole-person care. When you seek sports-medicine treatment for a running injury, demand that your clinician examine your whole body.
The best sports medicine care and, indeed, the best running addresses the whole person! Endeavor to run this way, and when you need it, treat your whole system.
Call for Comments (from Meghan)
- Have you treated an injury with whole-person care, which led to addressing and treating other areas of the body?
- What pain do you feel now that you suspect could be related to an issue elsewhere in your body’s system?